
Having the thalassemia gene does not make you less marriageable
People are hesitant getting their daughters tested for fear that no one will marry them if their results are positive.
It’s not easy being a father when you know your child has a critical illness. I still remember the words of a thalassemia patient’s father when we were in search of a blood donor for his son,
“Doctor Sahiba, log to meri shakal dekh ker hi munh pher lete hein ke phir aagaya hamara khoon nikalwane.”
(Doctor, now when people look at me, they turn away, thinking that I’m back again to ask for blood.)
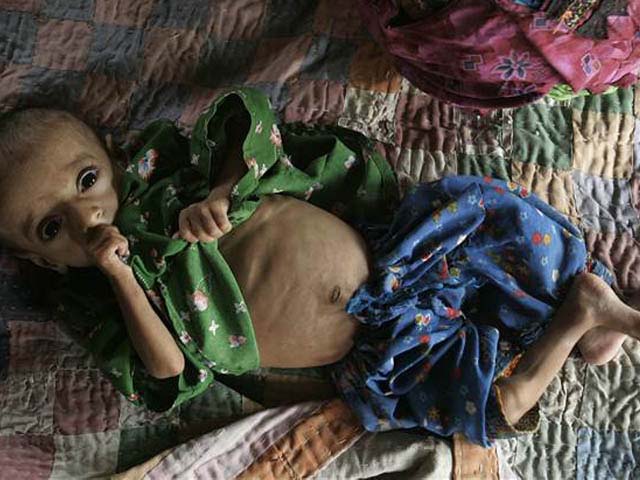
It’s the same story with Ahsan, a four-year-old child diagnosed with thalassemia at the age of six months. His treatment initially began with blood transfusions every three months which soon turned into monthly transfusions. And now, Ahsan has been getting weekly blood transfusions for the last three months.
We cannot even begin to imagine what his family goes through as they try to arrange blood for him. Since his parents are carriers themselves, they don’t have viable haemoglobin to donate blood to their own children and are forced to ask friends and relative for blood donations each time. Searching for rare blood groups such as O-negative, A-negative and B-negative adds to their miseries. While people don’t mind donating blood once or twice, donating blood on a regular basis requires a tender heart.
Have you ever been to a thalassemia centre? Have you seen the misery and pain of the patients? If you ever had the opportunity to visit, you must have seen pale children with hands swollen due to repeated intravenous canulation and blood bags hanging over their heads.
Unfortunately, patients suffering from thalassemia are increasing day by day in Pakistan. Although the government and social welfare societies try to help these children, it is impossible to accommodate them all due to limited resources. Bone marrow transplant is the only curative treatment available currently but not all patients can opt for it since it is very expensive.
Thalassemia is a life-long disease and keeping it under control is difficult. Beta-Thalassemia, a blood disorder that reduces the production of haemoglobin, poses an increased burden on our health system. It is impossible to provide blood transfusions and Iron Chelating Therapy – removal of excess iron from our bodies with the help of medicines – to all patients with such a limited health budget. Therefore, preventive strategies have to be looked into.
In Pakistan, approximately 5,000 children are diagnosed as thalassemia-major every year. In order to curb the rise of new cases, preventive strategies should be implemented before it is too late. The simplest way to keep an eye on potential cases and prevent them is to check the gene pool of diagnosed children’s families and avoid inter-family marriages of positive carriers.
Nowadays, hospitals provide tests to detect thalassemia in pregnant women to find out if the child is at risk of having the disease. The rate of thalassemia cases has decreased in Cyprus and Greece ever since these strategies have been implemented.
There is a dire need to educate people regarding screening programmes due to their lack of knowledge on such issues. Hence, we carried out a study regarding detection of thalassemia carriers at our hospital and offered genetic counselling accordingly. Unfortunately, the response we got from relatives of the diagnosed patients was not as good as expected. Even though the tests cost around Rs2,500 and were provided free-of-cost by the hospital, family members were not keen on getting the screening done. Parents and family members of girls, especially, were hesitant to get their daughters screened out of fear that no one would marry them if their results came out positive.
The social welfare officer at our hospital informed us that many children were registered with them and that the cost of transfusion was roughly Rs3,000 per transfusion. In addition to the monetary cost, they faced many problems while trying to arrange blood for transfusions.
Although it is our ethical and moral duty to support these patients and their families, I feel that we must focus on preventive strategies in order to prevent new cases from appearing.
We need to educate people in Pakistan and provide awareness of thalassemia screening programs. The government should at least provide free-of-cost facilities for screening tests to the relatives of the diagnosed child. Even though our government spends a huge fraction of the budget for the management of thalassemia, it’s not possible to facilitate all the patients. Hence, the government must focus on preventive strategies which are feasible and can be carried out easily.
Proper counselling is needed to clarify the myths and fear associated with being a thalassemia carrier. Most families have seen or heard about the misery, pain and stress the family of a diagnosed patient endures. I hope this exposure, along with counselling and awareness programmes will help motivate other people to opt for screen tests and reduce the risk of spreading the disease.
Ultimately, a national policy for the prevention of thalassemia is essential. The government needs to introduce easy and cost effective methods to detect the illness at an early stage and decrease the rate of this genetic disease.
And as individuals, we can all play our part by donating blood whenever possible. Donating blood is as good for the person giving it as it is for the receiver and can help reduce the risk of heart attacks and cancer, reduce iron levels which can thicken blood and increase free-radical damage and help reduce weight since donating a pint burns around 650 calories.
As with all diseases, awareness is key to fighting thalassemia. So, keep yourself informed and help others gain awareness too.
Who knows, you might end up saving lives.



COMMENTS (17)
Comments are moderated and generally will be posted if they are on-topic and not abusive.
For more information, please see our Comments FAQ